Call: (217) 762-4366
Request AppointmentGeneral Dentistry
Dental Exam
There's nothing to fear with a dental exam. Your teeth will be visually examined for signs of plaque, tartar and tooth decay. Your gums will also be examined for puffiness or discoloration, which are signs of gum disease. A full set of dental X-rays may also be taken during your dental exam, to enable your dentist to see below the surfaces of your teeth. Dental exams typically end with a dental cleaning, to remove surface stains and buildup.
Digital Dental X-Ray
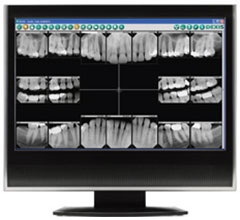
In our office we use digital radiography which allows us to take X-rays using 50-70% less radiation than conventional X-rays. Did you know that a digital X-ray contains the same amount of radiation as watching your TV for five minutes? Digital X-rays and computer technology allows us to enhance the images for better diagnosis of any dental concerns. X-rays are a necessary part of the diagnostic process, and not to use them could lead to undiagnosed disease. Without an X-ray of the whole tooth, and supporting bone and gum tissues, there is no real way to detect infection or pathology that requires attention.
Teeth Cleaning
Our office has two full-time hygienists and several part-time hygienists who provide experienced, exemplary service. It is recommended that patients schedule regular cleanings every six months to ensure the continued health of their teeth and gums. Some individuals may need personalized treatment plans with more frequent visits. In fact, research has shown that patients who have had gum surgery to treat periodontal disease can best maintain the health of their gums if they come every two to three months.
Oral Cancer Screening
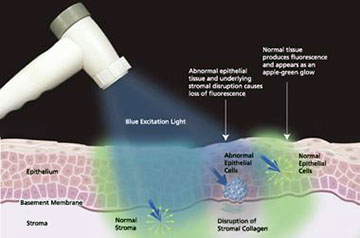
Oral cancer affects nearly 35,000 Americans every year. The keys to surviving oral cancer are early detection and early treatment. This starts with a regular oral cancer screening – at least once every six months. An oral cancer screening takes just minutes, is pain-free and can be performed during regular dental exams. If you are male, a regular oral cancer screening is especially critical: Oral cancer is more than twice as common in men as it is in women. Other people at high risk of oral cancer include people over the age of 60, tobacco smokers and heavy drinkers.
Dental Fillings
If you've been told you need a dental filling, you're not alone: 92% of Americans have had at least one cavity. Dental fillings are the tried-and-true treatment for treating cavities – and they come in a variety of options to suit every need. Dental fillings can be made of silver amalgam, composite, porcelain and even gold. Amalgam fillings have been used by dentists for more than a century and are still the most common and cost-effective type of dental filling. But composite fillings, which are made of a tooth-colored plastic and glass composite, are quickly becoming the preferred dental filling due to their natural appearance and durability. The type of dental filling used is determined by a number of factors, including size and location of the cavity, as well as your budget.
Tooth Colored Fillings
When a tooth has a cavity, the best treatment option is a filling. Caught early enough, cavities can be treated easily with little or no discomfort. If not treated decay can lead to tooth pain and/or infection, and the tooth would need root canal treatment or an extraction.
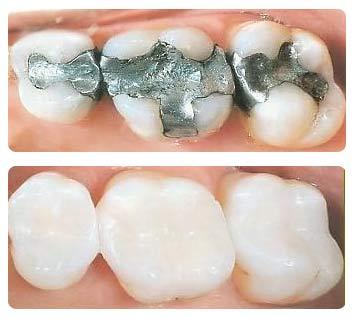
There are two types of fillings, amalgam (silver) fillings and resin (tooth-colored) fillings. These days most teeth are treated with bonded tooth-colored composite resin fillings. Most dentists prefer tooth-colored fillings because they bond to the tooth structure and therefore help strengthen a tooth weakened by decay. White fillings are also usually less sensitive to temperature, and they also look better. In certain situations, however, silver fillings may be more suitable because they are easier to place: there are fewer steps and it is not required that the area surrounding the tooth be kept dry while the filling is being placed.
The process for tooth-colored fillings is fairly simple. First, all of the decay is removed from the tooth. Then the surface of the tooth is roughened in order to accept the bonding and hold it. A gel is applied to micro etch the tooth surface, and a primer/bond agent is applied so the material adheres to the surface. The filling material is placed on the tooth and hardened with intense light. Finally, the filling is shaped and polished to get a lustrous finish as a last step.
Dental Crowns
A crown, or cap, is a man-made cover that is used to restore and preserve decayed, broken, or cracked teeth. Crowns are made out of several materials, including metal crowns, usually made of gold, and tooth-colored crowns usually made up of porcelain. Metal crowns are stronger but less aesthetically pleasing. We generally use combination crowns: tooth-colored porcelain fused to a metal base. This gives the patients the look of a natural tooth and the strength of a metal crown. Crowns are custom fit to your mouth and we have an extensive shade guide to ensure your crown matches the color of your natural teeth.
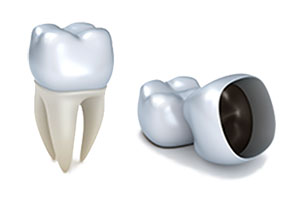
• A decayed or damaged tooth
• A cracked or broken tooth
• A poor-fitting crown
• A tooth that has a large opening due to root canal therapy
• A cosmetic or bite problem
The procedure for getting your tooth crowned requires two visits, usually with two weeks between visits. During the first visit, we will prepare the tooth, removing any decay and shaping the tooth to ensure the proper fit of your crown. We will then take an impression of your mouth that will be sent to the lab where they will craft your permanent crown.
We will place a temporary crown on the prepared tooth. A temporary crown acts like a Band-Aid, protecting your tooth from sensitivity. It is important to note that, while we shape the temporary crown to fit your mouth, it is not the same shape, color, or texture as your permanent crown. It is important that your temporary crown remain in place so please be careful. Don’t eat hard or sticky foods, brush gently, and remove floss from the side. If your temporary crown falls off, please call our office right away so we may schedule you to have it re-cemented.
During your second visit, we will remove the temporary crown and try in your permanent crown to be sure it fits properly. Once we are satisfied that the fit, bite, and color of the permanent crown are correct, we will cement it in place.
Porcelain Dental Crowns
Although dental crowns can be made of a variety of materials, including stainless steel, gold and silver, nothing looks better than a porcelain dental crown. Porcelain dental crowns match the natural color of your teeth and are virtually undetectable by the naked eye. And because they're metal-free, porcelain dental crowns are an excellent option for patients with metal allergies. Best of all, porcelain crowns don't just look beautiful – they're long-lasting, too!
Dental Bridges
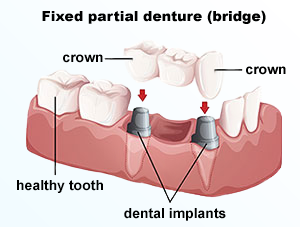
It is important to replace a missing tooth because the spaces left by missing teeth can cause your remaining teeth to shift, changing your bite and affecting your smile. If your bite is affected, your jaw may become sore and your teeth may be harder to clean leading to tooth decay and gum disease.
The procedure for getting a bridge is similar to that for a crown. There are two visits, one visit to prepare the tooth, take an impression of your mouth, and to fit a temporary bridge, and a second visit, two weeks later, to cement in your permanent bridge.
Dentures
While it is always best to try to restore and keep as many of your natural teeth for as long as possible, in some cases full dentures are a necessary solution. Dentures are made from strong gum-colored acryllic with acryllic teeth and are made to custom fit your mouth.
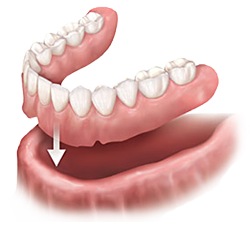
Benefits of full dentures include:
- Restoring your smile
- Providing support for the cheeks and lips filling out the appearance of your face and profile
- Improving your ability to eat a normal diet
- Improving your ability to speak clearly
If you and your dentist agree that full dentures are the best option for you, there are several steps to the process. In most cases, the first stage is to extract the remaining teeth. This is done in stages, working with one portion of your mouth at a time to allow your mouth time to heal after each visit, leaving the front teeth for the last visit.
When all of your teeth except for your front teeth have been removed and the gums have had several weeks to heal, we will take an impression of your mouth and send it to the lab so your dentures will be custom made to fit your mouth. Then once your dentures are ready we will remove the remaining front teeth and give you your denture so you will never be without a proper smile.
Even though your dentures are custom made to fit your mouth, it is not uncommon for minor adjustments to be needed within the first few weeks of obtaining your new denture. If your dentures are rubbing or causing sore spots on your gums, your dentist can quickly adjust them so that they are no longer a source of irritation. Never try to adjust or repair your dentures yourself.

Once your gums have healed after about three months, then your dentures will need to be relined so that they fit properly in front as well as in back. Your dentures will need to be relined or replaced every five to ten years in order to ensure that they continue to fit and function as they should.
When you first get your dentures they may feel awkward. Until you are used to your dentures it is best to eat soft foods cut into small pieces chewing with both sides of your mouth at the same time. It is also a good idea to read out loud to get used to speaking with your dentures in place.
Denture Care:
- Thoroughly rinse away all food debris after each meal.
- Brush your dentures at least twice a day with a denture brush using denture cleanser or mild soap.
- Be sure to handle your dentures over a folded towel or a sink full of water to prevent damage if dropped.
- Soak your dentures in denture cleanser every night.
- Do not allow your dentures to dry out as they may change shape. When you are not wearing your dentures, soak them in denture cleanser or in cool water. Never use hot water as it can cause your dentures to warp.
- Be sure to continue to take care of your mouth. Brush your tongue, gums and palate at least twice a day to remove plaque and stimulate circulation.
Partial Dentures
A partial denture, often referred to as a partial, is the most common solution to replace missing teeth. Partial dentures consist of acryllic replacement teeth, gum-colored acryllic, and metal clasps to attach the partial to your remaining teeth. One advantage of a partial denture is that teeth can be added to it at any time. Partial dentures are a relatively inexpensive option to replace several missing teeth as long as the remaining teeth provide adequate support. Some partials have no metal support and can quickly be converted to a full denture if necessary.
If you decide that a partial denture is the best option to replace your missing teeth, you will have to make several simple and quick visits to our office. The entire process typically takes about three weeks.
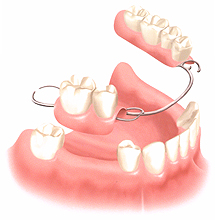
A partial denture is custom made to fit your mouth and you should be able to put it in and take it out without any trouble. However, your partial may still need to be adjusted by your dentist especially as your teeth shift over time. Never try to force your partial in or bite down to try to get it into place and never try to adjust your partial yourself.
Partial Denture Care:
- Rinse your partial after eating.
- Brush your partial at least once a day over a folded towel or a sink full of water so that if you drop your partial it won’t be damaged.
- Use a soft denture toothbrush and soap or denture toothpaste. Do not use regular toothpaste. Do not use bleach.
- Soak your partial in denture cleaner at least three times a week to prevent staining and odor.
One disadvantage of partial dentures is that food can get caught beneath them so you will have to take them out and clean them after every meal. Another disadvantage is that partial dentures are made with metal clasps which may be visible when you smile or speak.
We also offer DuraFlex Flexible Partial Dentures.
Gum Disease Treatment
Non-surgical gum treatments, such as deep cleaning, scaling, and root planing, are used to treat patients who have gum disease. The gums, ligaments, and bone surrounding the teeth are all important for the overall health of your mouth.
Periodontal Disease:
Periodontal disease is a broad term used to describe various diseases that affect the gums, bone, and surrounding structures of the teeth. The most common types are gingivitis and periodontitis. Gingivitis is the inflammation of the gum tissue caused by the accumulation of plaque and tartar that leads to bleeding and reddening of the gums. Periodontitis damages the bone and connective tissue that support the teeth. If left untreated, periodontitis can lead to tooth loss.
Risk Factors:
- Poor dental hygiene, poor nutrition, smoking, or chewing tobacco
- Poorly contoured fillings or crowns
- High levels of stress
- Medical conditions such as diabetes, down’s syndrome, AIDS
- Medications such as steroids, oral contraceptives, and blood pressure medications
Warning Signs and Symptoms:
- Red, puffy, swollen, or tender gums
- Bleeding when you brush or floss
- Itchy sensation
- Teeth that are loose or shifting, changes in your bite or in the fit of your partial denture
- Tooth sensitivity
- Gum recession
- Constant bad breath or a bad taste in your mouth

- Proper brushing and flossing
- Balanced diet to supply important nutrients and plenty of water to increase saliva
- Regular dental visits
If you show symptoms of periodontal disease, your dentist or hygienist will give you an evaluation using a periodontal probe to measure the space between your teeth and gums and take x-rays to determine if there is bone loss.
The main treatment for periodontal disease involves a deep cleaning. A deep cleaning includes scaling, scraping the tartar off the crown and root of the tooth, and root planning, smoothing the rough surfaces of the root removing the bacterial toxins which have coated the surface of the root and allowing the gums to better adhere to the root of the tooth and heal properly. This deep cleaning is usually done in stages, either one quadrant or one half of your mouth at a time.
For areas where the depth of the periodontal pockets are not adequately decreased by scaling and root planing, further treatment includes a localized antibiotic therapy and perhaps periodontal surgery. In some cases, more advanced surgery may be necessary in order to treat the disease.
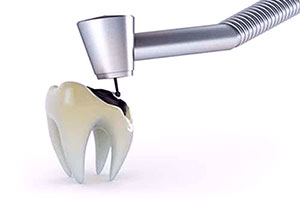
Endodontics
Root Canal Therapy is a treatment used to save teeth that are severely damaged and have an infection in the nerve chamber of the tooth. In the past, these teeth would have needed to be extracted but with modern dental techniques, 90% of damaged teeth can be saved. If left untreated the infection will spread, leading to bone loss around the root of the tooth and further health problems. Without this supporting bone structure, the tooth will become loose and fall out. Infected teeth are often painful so we recommend treatment as soon as possible after receiving a diagnoses.
Causes:
- Trauma, such as a physical blow to the face
- Abscessed tooth
Symptoms:
- Symptoms of an abscess tooth, such as sensitivity to hot or cold, discomfort while biting, or throbbing pain that disrupts normal sleep
- Discoloration (tooth turns gray)
We will talk with you about your symptoms and take an X-ray of the area before giving you a diagnosis. The root canal procedure itself usually takes only one visit. During that visit, the diseased nerve tissue will be removed and the root canals will be cleaned out and then filled with a rubber-like material. We will then place a filling to cover the opening in your tooth.
We highly recommend that any root-canal treated teeth be crowned, to ensure the continuing health of your tooth.
Extractions
If a tooth is severely decayed to the point that a restorative treatment cannot be attempted, it may be necessary to have that tooth pulled. Sometimes having your tooth extracted is the only treatment option. It is usually a comfortable and efficient procedure.
Our office also performs wisdom teeth extractions. If the tooth is erupted (above the gum line) it is a quick and simple procedure to have it removed. If the tooth is below the gum line Dr. Wintersteen will provide a referral to an oral surgeon to have the tooth removed.
Getting your tooth extracted is a simple process. We will provide you with anesthesia and check the area around to tooth before we begin the procedure to be sure that you are adequately numb. We will loosen the tooth and then remove it from the socket. In certain situations it may be necessary to cut the tooth in half and remove it in sections. During the procedure you will feel but you should not feel any pain. If you do, please let us know and we will give you more anesthetic.
TMJ Treatment
TMJ stands for temporal-mandibular joint. Temporal refers to the temple area of the skull and mandibular refers to the mandible, or lower jaw. This joint is where the head and jaw meet. Problems in this joint may be caused by a misalignment of the teeth, trauma, or excess muscle tension. Aside from the two bones that meet there, cartilage buffers them and five muscles are involved in the area. If something goes wrong a good deal of trouble can result.
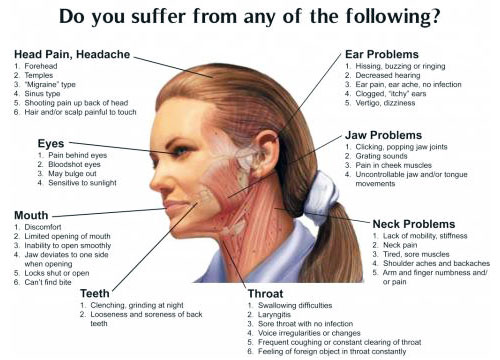
Problems in this area can cause:
- Headaches
- Earaches
- Trouble/soreness in opening and closing the mouth
- Clicking or popping of the jaw
- Pain in the jaw muscles
- Soreness in the area, sometimes extending to the face
Dental treatments for the condition can include replacing missing teeth, moving teeth, adjusting the bite, filling gaps between teeth, etc. There is no one solution that is right for all cases. Sometimes a plastic mouthpiece, such as an NTI, is used to prevent clenching or grinding that is contributing to the problem. If untreated and taken to extremes, surgery may be required to repair a badly damaged joint.
Pediatric Dentistry
Catering to the dental needs of kids requires a special touch. Pediatric dentists are specially trained to treat the oral health needs of children, from infancy through their teenage years. This involves in-depth knowledge about children's behavior, as well as their growth and development. Pediatric dental offices are also designed to make kids feel comfortable and relaxed – with plenty of toys, activities and a warm, inviting and fun décor.
NTI Migraine Headache Treatment
If you have jaw pain, a stiff or sore neck, morning headaches, tension headaches, or sensitive teeth (or any combination of these symptoms) you may be unknowingly grinding or clenching your teeth at night. The good news is that your dentist has a simple solution to treat this problem: an NTI.
An NTI (Nociceptive Trigeminal Inhibition Tension Suppression System) is a small device that fits over the front teeth (top or bottom). This device is generally worn only when you sleep and it prevents your back teeth from touching. The difference between the NTI and traditional mouth guards is that traditional devices, while they keep your teeth separated, still offer a surface to bite down on and can actually lead to clenching your teeth with even greater force.
The NTI addresses this problem because it does not allow your back teeth to touch at all which greatly reduces the pressure which you can exert while clenching or grinding. The reflex to clench or grind your teeth at night is suppressed.
Most patients notice improvement within a few days with maximum results typically obtained within 8 week. In fact, here at Dr. Wintersteen’s office, if you are not satisfied with your NTI, we will give you a full refund and therefore the NTI is a risk-free treatment for your symptoms.
